Introduction
Biceps brachii injuries are the most common injury to the anterior elbow. Injuries to the brachialis muscle are rare but can occur with or without injury to the biceps brachii.1,2 In 2001 the first case report of brachialis muscle tear from lifting a heavy object was published.3 Because of the rarity of injury to this muscle and its conflicting morphology described below, diagnosis of brachialis injuries is a challenge.4
Anatomy of the Brachialis
The brachialis is a strong thick muscle on the anterior elbow and upper arm. It originates on the anterior distal half surface of the humerus and runs distally to attach on the proximal ulna at both the ulnar tuberosity and the coronoid process.5 Unlike some of the other anterior arm muscles who have multiple functions, the brachialis’ function is isolated to flexion of the elbow.6 Due to its large cross-sectional area (7 cm2) it is the greatest force generator at the elbow.7 The brachialis has been shown to provide up to 47% of elbow flexion torque.8 The brachialis may be responsible for elbow stability throughout both concentric and eccentric muscle function and is preferentially recruited over the biceps brachii when undergoing a strong eccentric contraction.9 Authors of classic textbooks have described the brachialis as having only one head,10 although others have disagreed, and feel that it may be divided into two heads; superficial and deep.11 And more recently, Piagkou and colleagues found a four-headed brachialis specimen.5 The brachialis muscle is innervated by the musculocutaneous nerve and some parts of the radial nerve, while branches of the brachial artery and recurrent radial artery provide its blood supply.
Brachialis injury typically occurs as repetitive overuse or acute trauma caused by hyperextending the elbow against resistance. The repetitive pull-ups in rock climbers, with the forearm in pronation may create a strain or tendinopathy of the brachialis known as “climber’s elbow.”12 There have been case study descriptions of injuries to brachialis in football, hockey, rugby, and while lifting weights heavy objects.1–3,13–19 Patients will typically complain of constant or intermittent anterior elbow and upper arm pain. There is rarely bruising or neurological injury with these muscle tears. Patients may notice a slight swelling in the anterior arm or cubital fossa. There will be some degree of weakness of elbow flexion depending upon the extent of injury; however, supination and pronation strength and range of motion should be spared. A loss of extension range of motion may be seen if symptoms are severe, for example in the case of bony avulsion.
The Role of MSK Ultrasound in Brachialis Evaluation
Advantages
-
Real-Time Imaging: Allows dynamic evaluation of brachialis integrity while the elbow and forearm can be moved through available range of motion.
-
High-Resolution Visualization: Provides detailed images of soft tissue structures, including the brachialis muscle and tendon fibers and their attachment to the enthesis.
-
Accessibility and Cost-Effectiveness: MSK ultrasound is portable, widely available, and less expensive than magnetic resonance imaging (MRI).
Limitations
-
Operator Dependency: Requires skill and experience for accurate interpretation of findings. The ability to sonograph is to a large extend influenced by the operator and the availability and technical considerations of state-of-the-art equipment.
-
Depth Limitations: Because of the superficial location of the brachialis, visualization is very effective, and depth does not seem to be a limiting factor for its examination.
-
Artifacts and Shadows: Bone and calcifications may create image artifacts, requiring adjustments in probe positioning and frequency.
Sonographic Technique for Evaluating the Brachialis
Equipment Setup
-
Transducer Type: Because of the medium depth of the brachialis, a high-frequency, linear array transducer is normally used.
-
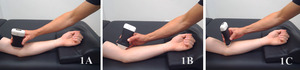
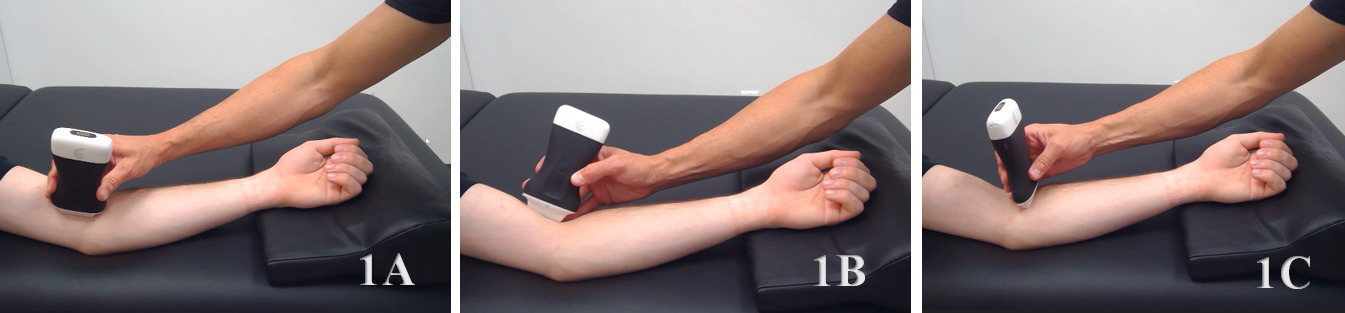
Patient Position: Patient is supine or seated with the arm resting on a pillow or supported on a table. The elbow is flexed slightly (20–30°) and forearm supinated to allow for better visualization of the brachialis deep to the biceps brachii. Adjust the arm position to allow optimal access to the anterior compartment of the upper arm.
-
Dynamic Assessment: Stress maneuvers, such as resisted elbow flexion or passive elbow extension, can be applied during MSK ultrasound to reveal tendon or muscle fiber disruptions, dynamic impingement of adjacent structures, or changes in echogenicity that may indicate tendinopathy or partial tears.
Examination Protocol
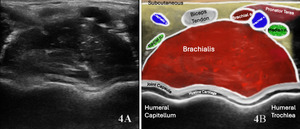
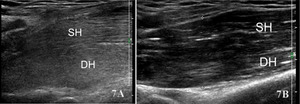
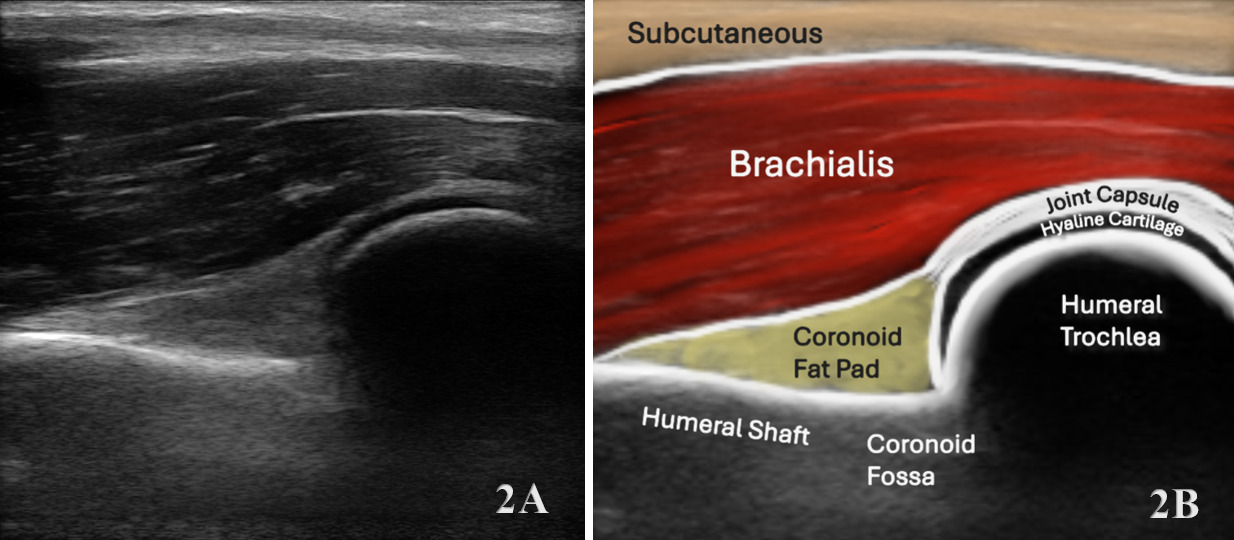
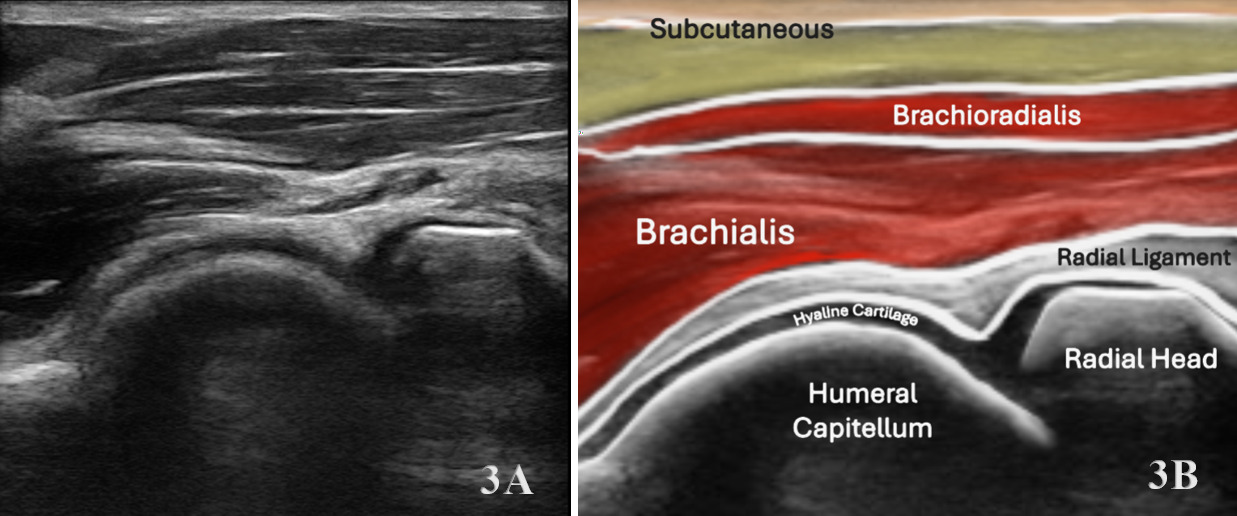
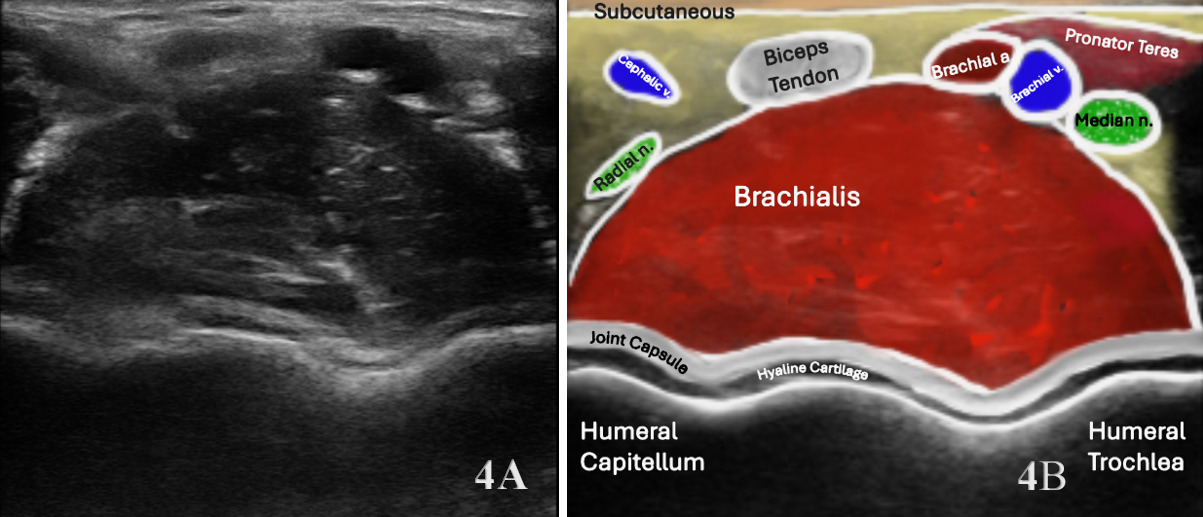
The brachialis is assessed using a linear high-frequency transducer (10–15 MHz), placed transversely over the distal anterior upper arm to identify the brachialis deep to the biceps brachii. In the short-axis (SAX) view, begin at the distal third of the humerus, visualizing the biceps superficially and the brachialis as a deeper, more hypoechoic structure adjacent to the humerus. Rotate the transducer 90° for a long-axis (LAX) view, tracing the muscle proximally toward the mid-humerus and distally to its insertion on the ulnar tuberosity.
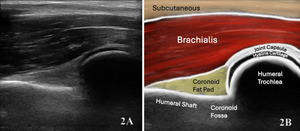
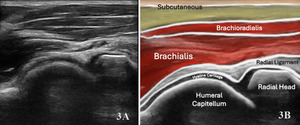
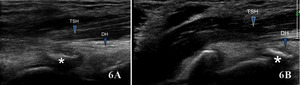
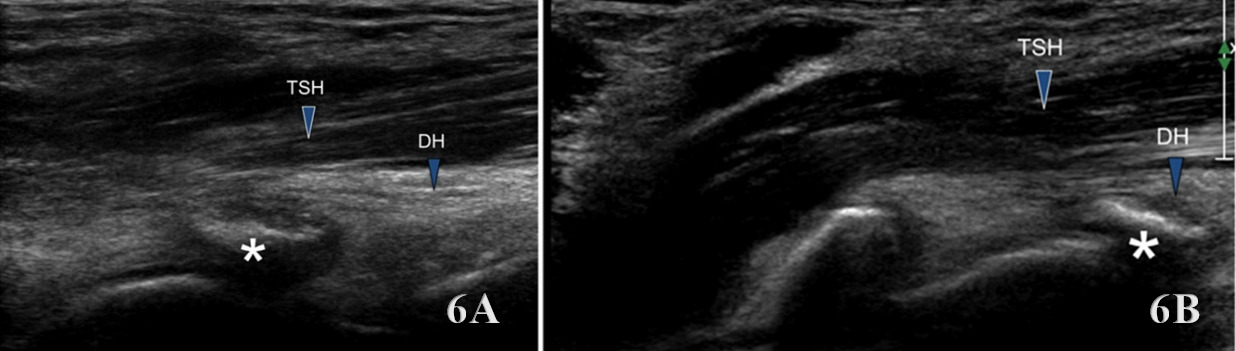
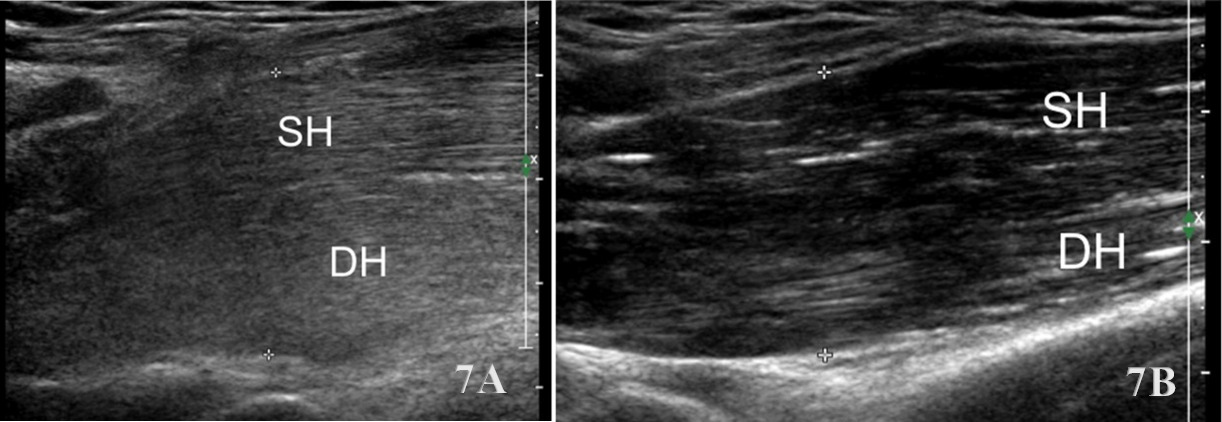
Normal Sonographic Appearance
Normally the brachialis tendon is viewed in both LAX and SAX views. The brachialis tendon can be seen distally at the ulnar attachment. The hyperechoic outline of the ulna will be seen below the brachialis. The brachialis tendon will be more hyperechoic in appearance, while proximally from the ulna the brachialis muscle will be hypoechoic tissue. In the LAX view the muscle should be fibrillar. The soundhead may need to be toggled at the distal tendons insertion to avoid anisotropy. Dynamic visualization can be performed with resisted elbow flexion and forearm pronation and supination.20,21
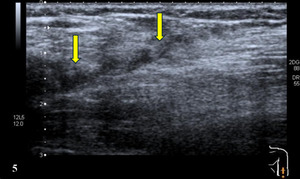
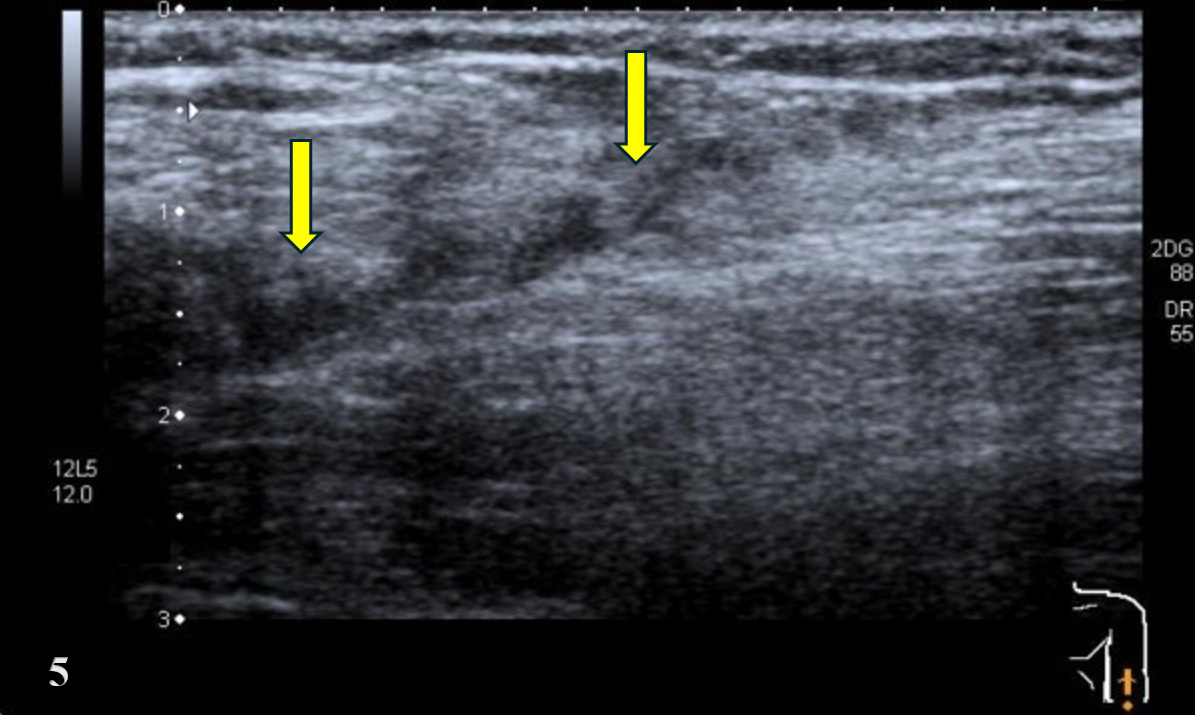
Pathologic Findings in Brachialis Injury
-
Hypoechoic thickening due to swelling and edema
-
Disruption of fibrillar pattern in partial tears and ruptures
-
Cortical irregularity and interruption in bony avulsions of insertion
-
Associated edema and effusion
Clinical Implications for Rehabilitation Providers
MSK ultrasound provides real-time feedback for rehabilitation professionals, facilitating early diagnosis and intervention. Key applications include:
-
Early Detection of Injury / Accurate Injury Grading: MSK ultrasound can help guide treatment planning by quantifying muscle injury, tendinopathy, and bony avulsion of the insertion
-
Dynamic Functional Testing: Rehabilitation professionals can use MSK ultrasound during physical therapy sessions to monitor recovery and assess muscle function dynamically. Serial MSK ultrasound imaging aids in assessing tissue remodeling, thickness and readiness for rehabilitation progression.
- Guided Interventions: Ultrasound imaging assists in precision-guided injections, such as corticosteroids for inflammation.
- Patient Education: Real-time imaging serves as a visual aid to explain the nature of the injury and set realistic expectations for recovery.
Limitations and Challenges
Despite its advantages, MSK ultrasound cannot entirely replace MRI for complex elbow and forearm cases. Additionally, the expertise required for optimal imaging technique limits its immediate adoption across all rehabilitation settings.
Conclusion
Diagnostic MSK ultrasound is a valuable tool for the evaluation of the brachialis injuries of the elbow and upper arm, offering fast, accurate, and cost-efficient imaging for rehabilitation professionals. Its ability to provide real-time, dynamic assessments makes it particularly suited for rehabilitation providers who can integrate the MSK ultrasound findings into clinical decision-making, optimizing treatment strategies and improving patient outcomes. However, practitioners must be adequately trained to maximize its diagnostic potential. By integrating MSK ultrasound into practice, rehabilitation providers can enhance patient care, improve outcomes, and reduce the burden of false diagnoses or delayed treatment.
Patient Positioning
The patient is positioned seated or supine with the arm resting in a supinated or neutral position, elbow slightly flexed (approximately 20–30°) to place the brachialis muscle under mild tension. A towel roll or pillow under the forearm may help stabilize the limb for optimal imaging.