Introduction
Hamstring injuries may be among the most common injuries to the posterior thigh muscles in young, active individuals. All of the hamstring muscles attach proximally to the ischial tuberosity.1 These injuries typically occur when the muscle goes through an eccentric contraction as part of dynamic movement, like sprinting or kicking, and is injured at the proximal myotendinous junction.2,3 The late portion of the swing phase of sprinting appears to be the most vulnerable position for the biceps femoris as the hamstrings produce a violent eccentric contraction to decelerate the forward-moving tibia.4–7
Anatomy of the Proximal Hamstring Tendons
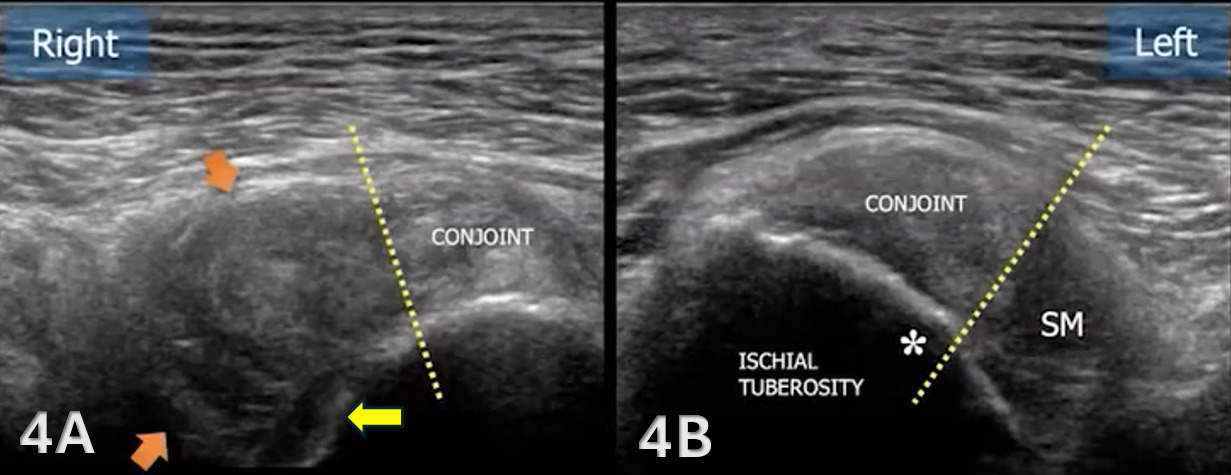
The proximal medial hamstrings consist of both the semitendinosus and semimembranosus, and the proximal lateral muscle, the biceps femoris, all of which originate on the ischial tuberosity.8 The biceps femoris long head and the semitendinosus muscle originate from a conjoint tendon at the medial posterior aspect of the ischial tuberosity, while the semimembranosus attaches more laterally and anteriorly.9,10
The hamstring tendons and muscles are surrounded by connective tissue, including the fascia lata and the ischio-gluteal bursa, which reduce friction during hip extension and knee flexion. This proximal portion of the biceps femoris attachment and configuration allows the hamstrings to play a key role in generating powerful hip extension, controlling knee flexion, and stabilizing the pelvis during gait and athletic activity.11
The Role of MSK Ultrasound in Tendon and Muscle Evaluation
Advantages
-
Real-Time Imaging: MSKUS allows dynamic evaluation of all the proximal hamstring tendons while the knee can be manipulated through the available range of motion.
-
High-Resolution Visualization: MSKUS provides detailed images of the proximal hamstring tendons and their proximal enthesis at the ischial tuberosity.
-
Accuracy: MSKUS has been proven to be both a valid and reliable method for examining hamstring architectural properties at rest.12–15
-
Accessibility and Cost-Effectiveness: MSKUS is portable, widely available, and less expensive than magnetic resonance imaging (MRI).
Limitations
-
Operator Dependency: MSKUS requires skill and experience for accurate interpretation of findings. The ability to sonograph tendons and their respective muscles is largely influenced by the operator and the availability and technical considerations of state-of-the-art equipment.
-
Depth Limitations: Visualization is usually not a problem; however, in some individuals, a curvilinear probe may be indicated due to depth.
-
Artifacts and Shadows: Bone and calcifications may create image artifacts, requiring adjustments in transducer positioning and frequency.
Sonographic Technique for Evaluating the Proximal Hamstrings
Equipment Setup
-
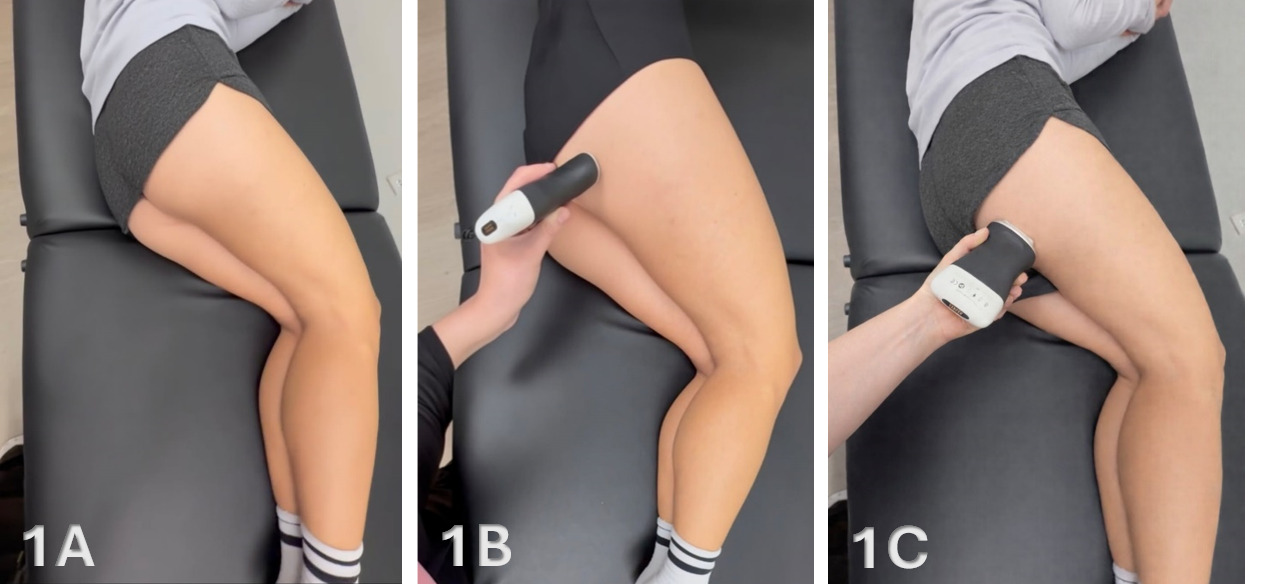
Transducer Type: Because of the depth of the proximal hamstring tendon and muscle, a standard high-frequency, linear array transducer between 5-15 MHz is normally utilized. However, in some individuals with more adipose tissue or larger muscle mass, depth may require a lower-frequency curvilinear probe to obtain depth.10,15,16
-
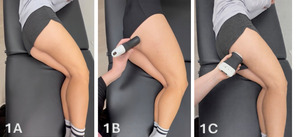
Patient Position: The patient is in sidelying with the knees and hips slightly flexed, or in the prone position with the feet over the edge of the table.
-
Dynamic Assessment: A passive or active movement of knee flexion and extension can be applied during ultrasound assessment to evaluate for proximal hamstring contractile and excursion properties.
Examination Protocol
Normal Sonographic Appearance
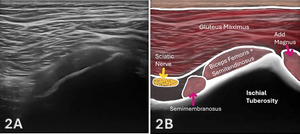
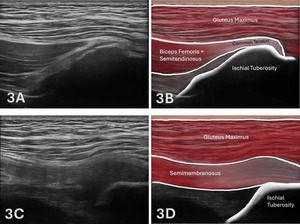
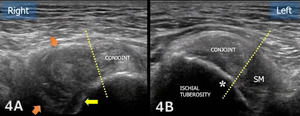
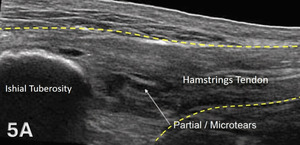
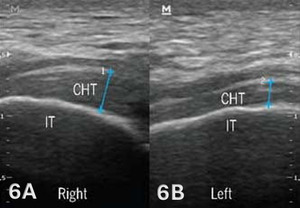
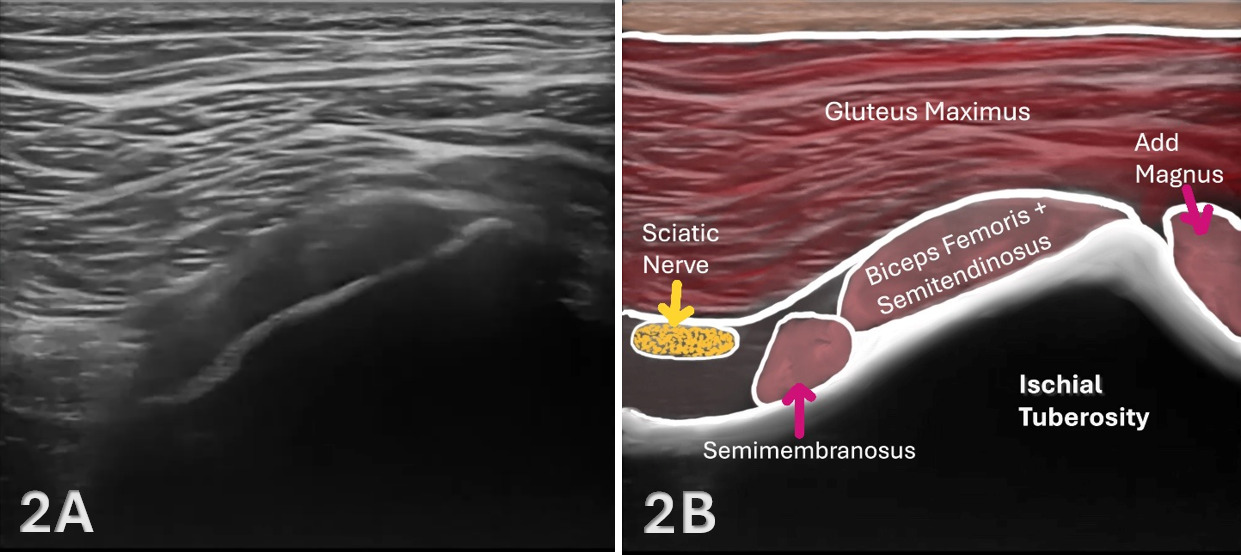
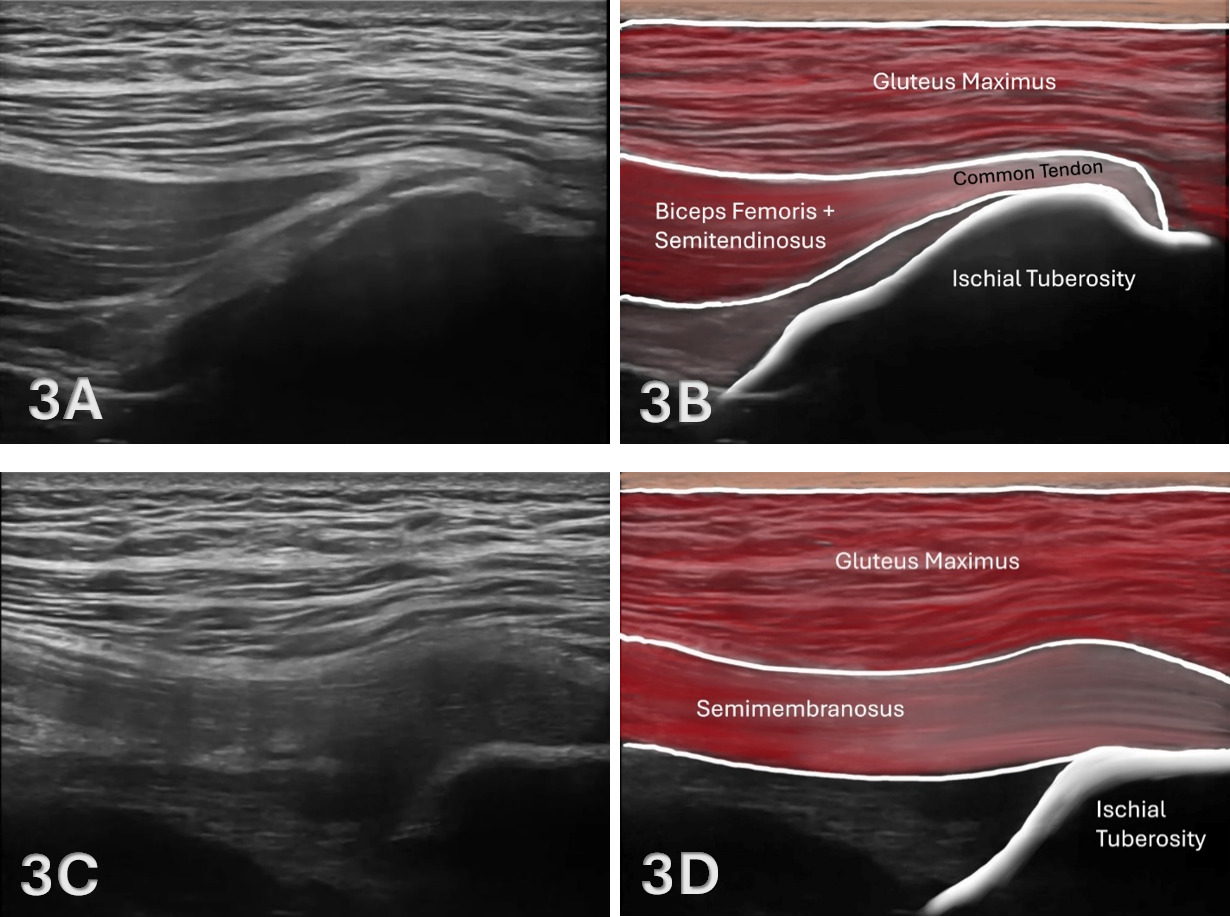
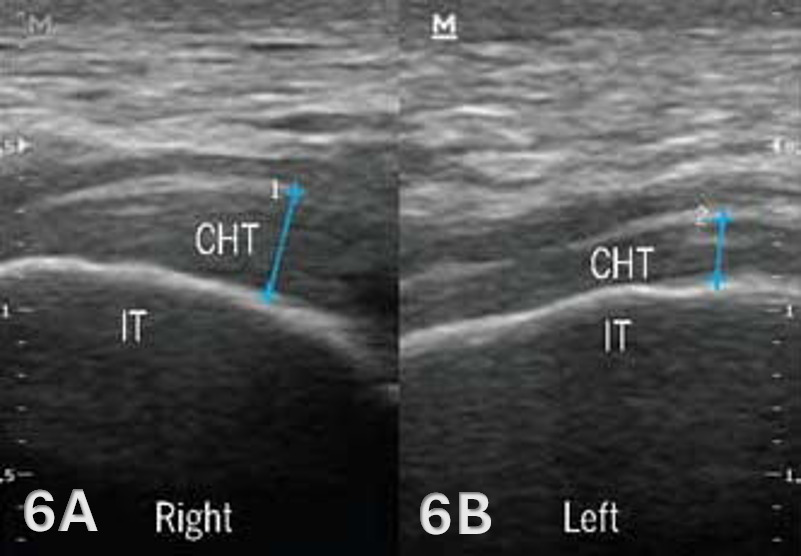
The starting point for examining the proximal hamstring tendon and muscle is at the osseous landmark – the ischial tuberosity.12,13,17–19 The ischial tuberosity can almost always be palpated, giving the examiner a perfect location to begin their scan. The proximal hamstring can be scanned in both the long axis (LAX) and the short axis (SAX). In the LAX view, depending on the probe width and size, one should start proximally to visualize the hyperechoic reflection of the bony cortex of the ischial tuberosity, with its large acoustic shadow underneath. In LAX, the proximal hamstring tendon fibers of the long head of the biceps femoris and the semitendinosus conjoint tendon should be easily seen coming off the attachment of the ischial tuberosity with a clear hyperechoic fibrillar structure running distally from the insertion site on the anterior lateral origin of the ischial tuberosity. The semitendinosus fibers can be easily seen as they reach the ischial tuberosity directly. Lateral to the hamstring muscle complex, the sonographer will see the sciatic nerve that appears as a fascicular, flattened structure that descends between and deep to the long head of the biceps femoris and semimembranosus tendon.1 The probe can be turned 90 degrees for viewing in the SAX. If the probe is moved slightly distally in the SAX view, the biceps femoris will appear as a triangular shape. As the examiner moves distally along the biceps muscle belly, the size will decrease until it appears to disappear. In both views, some toggling may be required to reduce anisotropy.
Pathologic Findings in Lateral Proximal Hamstring Tendon and Muscle Injury
-
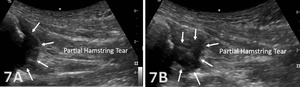
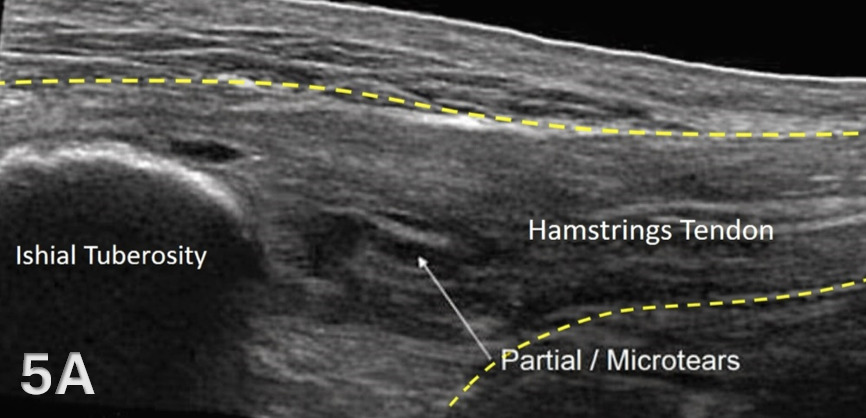
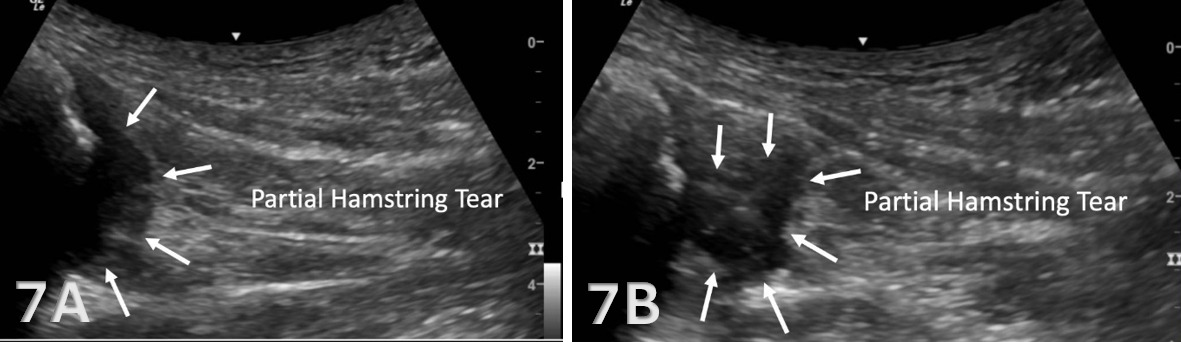
Disruption of fibrillar pattern in partial tears and ruptures. Proximally, it is important to determine if the injury is a free-tendon injury or purely a myotendinous injury.20
-
Associated effusion.
-
Calcifications of the tendon near the enthesis sites.
-
Bony avulsions and or retracted tendons from ruptures or avulsion fractures.2,21
Clinical Implications for Rehabilitation Providers
MSKUS provides real-time feedback for rehabilitation professionals, facilitating early diagnosis and intervention. Key applications include:
-
Early Detection of Injury / Accurate Injury Grading: MSKUS can quickly differentiate between a tendinopathy versus a strain, or more severe tendon rupture or muscle tear, to help guide treatment planning.
-
Dynamic Functional Testing: Rehabilitation professionals can use MSKUS during physical therapy sessions to monitor recovery and assess tendon and muscle function dynamically. Serial MSKUS imaging aids in assessing muscle healing and remodeling to help with readiness for rehabilitation progression.
-
Guided Interventions: Ultrasound imaging assists in precision-guided dry needling or injections, such as corticosteroids for inflammation.
-
Patient Education: Real-time imaging serves as a visual aid to explain the nature of the injury and set realistic expectations for recovery.
Limitations and Challenges
Despite its advantages, MSKUS cannot entirely replace MRI for complex cases, especially when examining the origin at the ischial tuberosity.22 Additionally, the expertise required for optimal imaging techniques limits its immediate adoption across all rehabilitation settings.
Conclusion
Diagnostic MSKUS is an increasingly valuable tool for evaluating proximal hamstring disorders at the ischial tuberosity, offering portable, real-time, high-resolution imaging that can improve diagnostic accuracy and confidence in rehabilitation and sports medicine settings. When paired with a sound understanding of proximal hamstring anatomy, typical injury patterns, and proper scanning technique, MSKUS can help clinicians differentiate tendinopathy, partial tears, and ruptures; monitor healing over time; and better individualize rehabilitation progression and patient education. Although MSKUS remains operator dependent and may not fully replace MRI in more complex presentations, its accessibility and ability to provide dynamic assessment make it a practical adjunct for guiding clinical decision-making and supporting optimal return-to-sport outcomes.