Introduction
The pectoralis major is at risk during any activity in which the arm is extended and externally rotated while under maximal contraction.1 The pectoralis major muscle, a powerhouse of the chest wall responsible for adduction, flexion, and internal rotation of the arm, is frequently exposed to high tensile forces during athletic activities. This vulnerability makes it susceptible to a spectrum of injuries, ranging from mild muscle strains to complete muscle or tendon ruptures. Accurate and timely diagnosis is crucial for guiding appropriate treatment and ensuring optimal recovery. Traditionally, magnetic resonance imaging (MRI) has held the position of the gold standard for diagnosing pectoralis major injuries.2,3 However, its limitations, including high cost, limited availability, and static imaging, have paved the way for the emergence of musculoskeletal ultrasound (MSKUS) as a compelling alternative.4–6 This article aims to provide rehabilitation professionals with an understanding of MSKUS in the context of pectoralis major injuries.
Pectoralis major muscle injuries usually occur secondary to weightlifting in nearly 50% of cases.7,8 The bench press is a common culprit due to the excessive tension put on an eccentrically contracted muscle as the bar is lowered to the chest. Less commonly, injuries occur after direct trauma causing forced abduction and external rotation of the upper extremity.6,9 Tendon tears occur almost exclusively in males between 20–40 years old and are heavily associated with anabolic androgenic steroid use.9–11 From a historical perspective, the first case of this injury was described in 1822 by Patissier in Paris involving a butcher boy who tore his pectoralis major in an attempt to lift a large piece of beef from a hook.4 The next several reported cases all involved men’s arms/shoulders being run over by horse-drawn carts.5 As athletic activities, particularly weightlifting and the bench press, increased in popularity toward the latter half of the 20th century, sports-related injuries began to outnumber job-related injuries and now account for the majority of all reported pectoralis major ruptures.5 The ability to detect and treat a pectoralis major rupture is important for both the clinician and the patient and is aided with knowledge of anatomy, the physical examination, and results of imaging studies. MRI has the ability to differentiate the site, grade, and chronicity of injury, it is expensive, time-consuming, while its availability is often limited to the hospital and/or emergency room setting.12 In contrast, point-of-care ultrasound (POCUS) is commonly available and can be used to help confirm the diagnosis and hasten disposition.2
Anatomy
The pectoralis major is a complex, fan-shaped muscle comprised of a clavicular head, originating from the medial half of the clavicle, and a sternocostal head, originating from the anterior sternum, costal cartilages of ribs 1–7, and the aponeurosis of the external oblique.2,13 The two heads come together and form a common tendon and insert into the intertubercular sulcus of the humerus.2,13 Rupture occurs most commonly in patients with a history of weightlifting, causing disruption of the distal humeral enthesis.7,14
Imaging
A variety of imaging techniques can be utilized in the assessment and management of pectoralis major ruptures. While these supplementary imaging modalities can aid in detecting a pectoralis major rupture, it is imperative to acknowledge that a physical examination is paramount in the identification of such tears, as imaging results can often be inconclusive or inconsistent. It is noteworthy that cases where imaging explicitly indicates a rupture are invariably corroborated by a physical examination. Consequently, although imaging studies contribute to the diagnostic process, the clinical examination should be considered the cornerstone of diagnosis.
MSK ultrasound offers a unique window into the intricate world of muscle and tendon pathology. By interpreting the characteristic features on ultrasound images, healthcare practitioners can accurately diagnose various pectoralis major injuries. In the context of pectoralis major ruptures, ultrasound has emerged as an efficacious and cost-effective diagnostic tool.15,16 It is advocated for its potential to expedite surgical intervention when a rupture is suspected.16 In practice, comparing ultrasound images of the uninjured side with the injured side can be particularly informative. An intact pectoralis major appears on ultrasound as a hypoechoic area, representing the muscle tissue, bordered by parallel echogenic lines indicative of the perimysium. The epimysium is discernible as a densely echoic layer anterior to the muscle. Any deviation from this pattern may suggest a rupture. Tears manifest as hypoechoic (darker) areas within the muscle belly, at the myotendinous junction, or at the humeral insertion. The disruption of the normal muscle fiber pattern is a telltale sign. Tendon abnormalities are characterized by thickening, disruption, or retraction of the pectoralis major tendon visualized on ultrasound suggest tendinitis, partial tears, or complete ruptures. Furthermore, ultrasounds are adept at identifying hematomas, which typically present as large, hypoechoic, well-defined entities within the muscle tissue itself. Therefore, ultrasound serves as a cost-effective and valuable alternative to MRI for the evaluation of pectoralis major ruptures.
Advantages of MSK Ultrasound
-
Real-Time Dynamic Assessment: MSKUS allows for the evaluation of muscle and tendon movements in real-time, crucial for assessing the pectoralis major.
-
High-Resolution Imaging: Enhanced image resolution aids in identifying subtle pathological changes within the muscle fibers and tendinous attachments.
-
Non-Invasive and Patient-Friendly: Unlike MRI, MSKUS is non-invasive, does not require exposure to radiation, and is generally more accessible and cost-effective.
Ultrasound Techniques for Pectoralis Major Evaluation
-
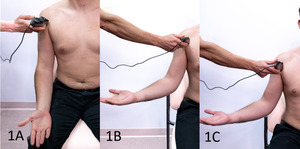
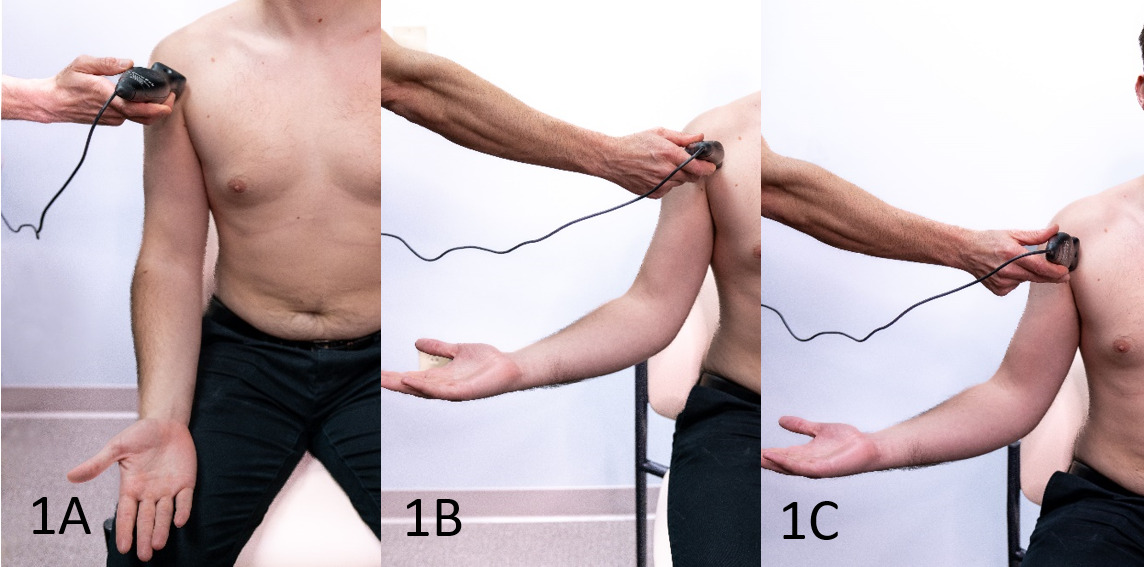
Transducer Positioning and Scanning Techniques: The article describes optimal transducer placement and scanning protocols for comprehensive visualization of the pectoralis major.
-
Identifying Pathologies: Techniques for identifying common injuries such as muscle strains, tears, and tendon avulsions.
-
Comparative Analysis: Emphasis on comparing the injured side with the uninjured side to identify discrepancies in muscle morphology and dynamics.
Integration into Rehabilitation Practice
-
Tailoring Rehabilitation Protocols: Utilizing ultrasound findings to customize rehabilitation strategies based on the specific nature and extent of the injury.
-
Monitoring Progress: The role of follow-up ultrasound examinations in monitoring the healing process and adjusting rehabilitation plans accordingly.
-
Patient Education and Engagement: Enhancing patient understanding and involvement in their rehabilitation journey through visual feedback from ultrasound imaging.
Conclusion: Prompt evaluation, radiographic confirmation, and surgical intervention are key in ensuring positive outcomes in active patients with pectoralis major tears. Diagnostic MSKUS represents a significant advancement in the evaluation of pectoralis major injuries. Its real-time, non-invasive nature makes it an invaluable tool for rehabilitation providers. However, its efficacy is dependent on the skill of the operator and should be seen as a complementary tool to a comprehensive clinical assessment.
.png)
.png)
.png)
.png)
.png)
.png)